July 9, 2016
Stanton A. Glantz, PhD
Accumulating evidence suggests e-cigs 1/3 to 1/2 as bad as cigs (maybe higher)
While e-cigarettes deliver fewer cancer-causing chemicals than conventional cigarettes, the evidence that e-cigarettes substantially increase heart and lung disease keeps piling up. This is important because heart and vascular disease (including stroke) and non-cancer lung disease account for over 70% of smoking-caused deaths. In addition, unlike cancer, where the dose-response effect for exposure to carcinogens is reasonably linear at the doses tobacco products deliver, the effects on cardiovascular disease are highly nonlinear, with the biggest increases in risk at the lowest doses.
Aruni Bhatnagar recently published a well-written (and cautiously interpreted) review of the evidence, “E-cigarettes and Cardiovascular Disease Risk: Evaluation of Evidence, Policy Implications, and Recommendations,” in which he observes
… cardiovascular tissues appear to be more sensitive to smoking than other tissues and organs. As a result, cardiovascular effects appear at levels of exposure lower than those required to cause other diseases, such as cancer. Moreover, recent analysis also suggests that the exposure-response relationship between smoking and CVD is non-linear. In this analysis, substantial risk was associated even with very light smoking. The curve rises steeply at low exposure levels and flattens out at higher levels, such that 80 % of the risk of smoking >20 cigarettes per day is associated with 50–80 % reduction in toxic constituents) might not significantly affect cardiovascular toxicity, even though the risk of other diseases (e.g., cancer) may be markedly reduced. In contrast, the dose-response relationship between smoking and lung cancer shows no threshold, and the risk is monotonically distributed. For those smoking >20 cigarettes per day, the risk of lung cancer death is >23 times higher than it is for non-smokers, while those who smoke one to four cigarettes per day have a 3-fold higher risk than non-smokers. Clearly, the mechanisms by which cigarette smoke causes heart disease and cancer differ. Moreover, even acute exposure to tobacco smoke can trigger adverse cardiovascular changes, whereas carcinogenesis requires more chronic exposure. … In addition, the increase in CVD risk due to smoking can be reversed more rapidly than cancer risk. The difference between the carcinogenic and cardiovascular effects of conventional cigarettes may be because the chemicals and constituents that cause heart disease are different from those that cause cancer or perhaps because cardiovascular process are more sensitive to cigarettes than the processes that cause lung cancer. Taken together, this evidence suggests that the relationship between smoking and CVD is fundamentally different from the relationship between smoking and cancer. This also suggests that the toxicants that cause cancer may not be the same as those that elevate CVD risk. From this, it follows that the cardiovascular effects of smoking cannot be assessed or predicted by knowing the chemicals and constituents that cause cancer. Hence, decreasing the levels of chemicals in cigarette smoke that cause cancer might not necessarily decrease CVD risk and might even increase or exacerbate cardiovascular injury. [emphasis added; references deleted]
He goes on to examine the effects of several chemicals in e-cigarette aerosol (including formaldehyde and acrolein) and has some nice graphs illustrating that the levels of these chemicals in e-cigarettes are at levels at which a variety of adverse effects occur. In particular, he notes, “even if the levels of acrolein in e-cigarettes are 10-fold lower than those present in conventional cigarettes, given the non-linear dose-response relationship between cigarette smoke and cardiovascular injury, it is not clear whether this would result in proportional harm reduction. Significantly, prolonged (90 days) exposure to even low-dose (0.2 ppm) acrolein results in non-specific inflammatory cardiac lesions. Hence, the generation of acrolein and other aldehydes in e-cigarette aerosols, even in low concentrations, remains a cause for concern.”
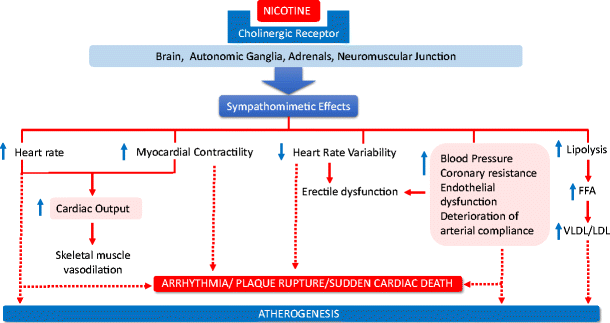
He also has an excellent discussion of the cardiovascular effects of nicotine in which he notes that the adverse effects of nicotine likely operate through complex changes in the nervous system that can affect blood vessels and the development of atherosclerosis, especially in the presence of other risk factors (see figure).
Based on the evidence as a whole, he concludes, among other things, that “E-cigarettes cannot be recommended as a safer alternative to smoking cigarettes.”
Nick Wilson and Coral Garter published a technical report summarizing the evidence on levels of biomarkers of effects on cancer, heart and lung disease published between January 2015 and March 2016. Based on their analysis, they concluded that e-cigarettes delivered about 10% of the amount of toxins for these diseases as conventional cigarettes (summary of report on their blog; full report). When they selected this level, they picked points in the middle of the available data; some of the studies showed higher levels. When interpreting their results, it is important to keep in mind the nonlinear nature of the dose-response for cardiovascular disease, so, as Bhatnagar points out, the effects are likely to be larger than the relative dose. Indeed, the levels of biomarkers of vascular effect in after using an e-cigarette vs. a cigarette they report from the study by Carnevale and colleagues shows smaller effects of e-cigarettes than cigarettes (but still substantial), whereas the e-cigarettes and cigarettes had the same effects on the physiological endpoint (ability of arteries to dilate).
Elizabeth Martin and colleagues published the results of a human study, “E-cigarette use results in suppression of immune and inflammatory-response genes in nasal epithelial cells similar to cigarette smoke,” whose title says it all. These effects, which were actually larger in e-cigarette users for some outcomes, are consistent with reduced ability to fight infections that lead to lung disease. They also highlighted volatile carbonyls, including formaldehyde, acrolein, and acetaldehyde, as possible reasons for these effects. These chemicals are produced by heating the propylene glycol and glycerin that are used as the primary constituents of e-liquids. Significantly, as coil temperature increases (with higher battery voltages) as is comment in the newer systems that are “more effective” at delivering nicotine, the production of these chemicals also increases.
So, what does this (and other) accumulating evidence mean in terms of overall risk of e-cigarettes?
One thing is for sure: The evidence-free “expert opinion” from group of e-cigarette enthusiasts that e-cigarettes are “95% safer” than cigarettes, which was repeated uncritically by Public Health England and the Royal College of Physicians is wrong. The longer these organizations take to modify their positions on the emerging science the lower their credibility is becoming.
Given the evidence that effects on the cardiovascular system and lungs account for more than half the smoking-induced deaths and that at least some of the short-term effects of e-cigarette use on these systems are comparable to cigarettes, agencies concerned about public health should consider them at least 1/3 as bad as cigarettes and maybe as high as half as bad (or higher).
And, that estimate if just for individuals using them, without accounting for the fact that e-cigarettes are attracting low risk kids and that kids who start with e-cigarettes are 3-4 times more likely to become cigarette smokers than those who don’t use e-cigarettes.

Add new comment