March 14, 2015
Stanton A. Glantz, PhD
Meta-analysis of all available population studies continues to show smokers who use e-cigs less likely to quit smoking
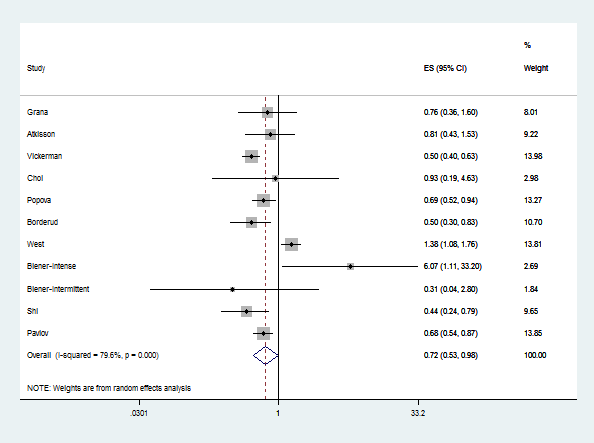 There are now 11 pubilshed studies that compare quitting smoking among smokers who use e-cigarettes compared to smokers who do not use e-cigarettes (counting the two analyses Lois Biener did, one for intense e-cigarette users and one for intermittent e-cigarette users, as separate estimates).
There are now 11 pubilshed studies that compare quitting smoking among smokers who use e-cigarettes compared to smokers who do not use e-cigarettes (counting the two analyses Lois Biener did, one for intense e-cigarette users and one for intermittent e-cigarette users, as separate estimates).
Using all these estimates in a random effects meta-analysis shows a significant drop in quitting with an odds ratio of 0.723 (with a 95% confidence interval ["margin of error"] of 0.531 to 0.983). Thus, smokers who use e-cigarettes are about 30% less likely to quit smoking than smokers who do not use-ecigarettes.
An interesting detail is that there is significant heterogeunity among the studies (p<.001 this="" heterogenuity="" is="" due="" to="" the="" brown="" study="" removing="" it="" from="" analysis="" makes="" test="" non-significant="" does="" not="" change="" overall="" conclusion="" pooled="" estimate="" of="" effect="" e-cigarettes="" on="" quitting="" just="" gets="" a="" little="" bigger="" ci="" p="" but="" raise="" question="" what="" different="" about="" study.="">

Comments
Thank you . . .
This appears to build on this: http://tobacco.ucsf.edu/e-cigs-can-increase-odds-smokers-using-them-quit... . Moreover:
<OL;
<LI;http://www.nytimes.com/2014/05/21/health/study-gives-e-cigarettes-edge-i...
“Stanton A. Glantz, a professor of medicine at the University of California, San Francisco, said the study’s limitation was that it tried to measure the effect of e-cigarette use only among smokers who were trying hard to quit, not all smokers.
Professor West responded that the study’s goal was to find out whether e-cigarettes helped people who were trying to stop smoking. But he said data still being analyzed may yet provide clues to the broader effects on smokers generally.”
Did Professor West ever come back about this further data analysis?
<OL;
<LI value="2";Clive Bates has stated that: “E-cigarettes <STRONG;provide a satisfactory alternative to smoking</strong; (nicotine, sensory and ritual aspects) and will displace cigarette use in the consumer market for recreational nicotine.” (Version 3 of his "E-Cigarettes, vaping and public health. A summary for policy makers"). This appears to be further misleading presumption from Clive: Do they? Professor Robert West himself here http://www.ft.com/cms/s/0/0c9307e0-ab91-11e4-8070-00144feab7de.html?site... is currently questioning that himself, due to his own most recent data here http://www.smokinginengland.info/latest-statistics/";http://www.smokingi... . In the FT article, he apparently stated along the lines of:</li;</ol;
“<EM;But although smokers are still using them as an aid to quitting, said Mr West, their popularity among continuing smokers has fallen as they find the devices do not always satisfy their nicotine cravings.”</em;
Significantly, Clive himself states very recently that:
“This is likely to be true”
here http://www.clivebates.com/?p=2838#more-2838";http://www.clivebates.com/?... , elegantly undermining his own previous claim with current evidence.
Dave Bareham
Moreover . . .
Here http://www.nytimes.com/2014/05/21/health/study-gives-e-cigarettes-edge-i... again, fascinating quotes emerge:
“Prof. Robert West, director of tobacco studies at University College London and senior author of the study, which is to be published Wednesday in the journal Addiction, said that clinical trials could not answer the question most people have about whether e-cigarettes help smokers quit because the devices are changing so fast that they become obsolete before an experiment ends. What is more, he said, people who wanted e-cigarettes and found themselves put in a group that used, say, the patch, would just drop out.
“The medical model is great for cancer drugs, but it doesn’t really work for this situation because there’s nothing to stop participants in the patches group from just going out and buying an e-cigarette,” Professor West said.”
If West (and significant others http://antithrlies.com/2014/09/25/why-clinical-trials-are-a-bad-study-me... in the “Harm Reduction” camp) believes that RCTs are not the appropriate methodology for analysing the effects of ENDS: then where does that leave the validity of the findings of the Cochrane Review carried out by West’s other ENDS-enthusiast colleagues (McRobbie, Hajek et al here http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD010216.pub2/abstra... )?
In this context, perhaps surprisingly, McRobbie et al included two underpowered RCTs in its analysis. In any case, as per the link, these researchers concluded that their confidence in their own “results” was either: “low” or “very low”, and this fact about the poor quality of data used is even confirmed by ECITA here http://www.ecita.org.uk/ecita-news/vapour-trail-latest-investigation-vap... in a “caveats” section. Clive Bates predictably makes no mention regarding these significant methodological issues and conclusions in his “Summary to Policy Makers” paper.
It’s been “fascinating” to see the in-house “debate/argument” on this issue of RCT develop, over recent months:
http://vapefight.com/casaa-says-not-to-contribute-to-dr-siegels-scientif...
http://tobaccoanalysis.blogspot.co.uk/2014/09/discontinuation-of-crowdfu...
<STRONG;i.e. the alleged “Divisiveness within the e-cigarette community” (Prof M. Siegel)</strong;
Dave Bareham.
RCT wasn't appropriate for NRT ueither
Why all the concern now over study integrity? Where were those concerns since Mooney et al 2004, which screamed that randomized placebo-controlled NRT trials were not blind as claimed as "subjects accurately judged treatment assignment at a rate significantly above chance." Although Mooney warned that "the validity of the results of clinical trials of nicotine replacement therapies could be questioned if future studies fail to assess the integrity of study blinding," that warning was ignored. How badly can blinding fail? Dar, Etter and colleagues found that control group members were 3.3 times more likely to correctly guess placebo than to incorrectly guess that they'd received nicotine (54.5% v. 16.4%). Jed Rose et al's prequitting nicotine patch study found that of 165 subjects receiving placebo patches, 27 believed they had received active patches, 112 believed they had not, and 26 were unsure."
A July 2013 Gallup Poll found that after 30 years of intense marketing that 1 in 100 ex-smokers credited nicotine gum for their success. If still unwilling to openly acknowledge OTC NRT's abject failure, and the consequences of 3 decades of teaching nicotine addicts that nicotine is medicine and its use therapy, imagine our starting point in attempting to objectively analyze newer forms of nicotine delivery.
Professors Siegel and Glantz are both deeply and genuinely committed to their advocacy. As I see it, nicotine dependency recovery is the victim. I sometimes wonder if either appreciates how their nicotine use advocacy plays directly to the addict's wanting for that next fix. Advocating different methods of introducting nicotine into the "quitter's" bloodstream, when does nicotine cessation get a turn?
In conflict with years of zealous replacement nicotine advocacy, it's my hope that Professor Glantz will at some point no longer fear teaching smokers the truth about how most ex-smokers succeed (abrupt nicotine cessation - cold turkey). In conflict with his e-cig harm reduction advocacy, it's my hope Professor Siegel at some point begins putting harm elimination first.
Gentlemen, ask yourself this. What is the key to successful abrupt nicotine cessation and can it be easily taught and shared? The most neglected cessation research issue is also the one offering the greatest potential to help end the addict's wanting for more.
John R. Polito
Nicotine Cessation Educator
another study gets much the same results
Summarized by Simon Chapman here:
https://theconversation.com/want-to-quit-smoking-switching-to-e-cigarett... title="https://theconversation.com/want-to-quit-smoking-switching-to-e-cigarett......
Addiction has yet to post onlline.
Jon Krueger
Add new comment